A common and distorted application of psychological safety is that it is somehow a shield from accountability. Non-performing employees tend to invoke it as an excuse for poor performance, insisting that a focus on psychological safety means valuing people and building relationships. That’s true, but stretching the premise, they claim that we should give them a pass when they don’t perform.
The flawed logic seems to be along the lines of because we may have used fear and intimidation, command and control, and manipulative and coercive tactics with people in the past, in an attempt to hold folks accountable, we must shed the artifacts that drive accountability in order to have an environment of psychological safety.
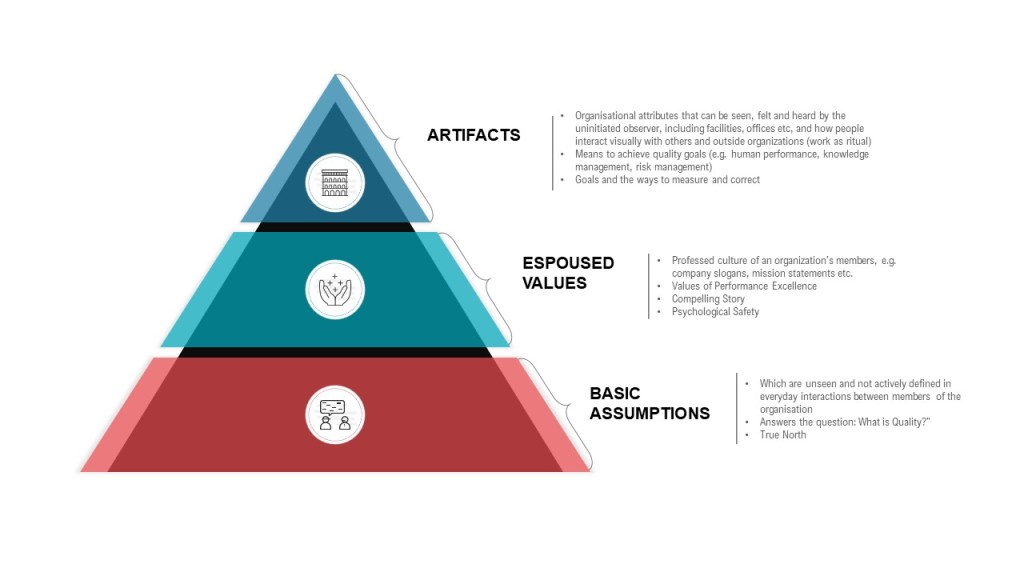
In my experience, this is especially prevalent when discussing metrics around overdue quality systems records and training. How to discuss what is late, can you even publish a list of folks with overdue training?
I want to be very clear, psychological safety is not a kind of diplomatic immunity from having to deliver results. It is not a shield from accountability.
Being held accountable can be looked at as transparency in progress. Psychological safety allows us to be vulnerable and to trust that the organization will take the problems seriously and address them.